How hand disinfection
came to be adopted
A brilliant 19th century physician made the connection between germs and disease
By Michael Walsh
August 12, 2020
How are you adjusting to the “new normal”? I am certain, like most of us, the three new methods of social interaction – distancing, masking and hand washing – have replaced behaviours learned since childhood. Unfortunately, it appears that these precautionary measures are destined to reshape society for an indeterminant period.
On a positive note, the current pandemic has changed one’s sense of thinking about the explosive nature of infectious diseases. Specifically, people now take an interest in public health and are cognizant that every individual has an important role to minimize viral contagion. More importantly, people understand how one infected person (“patient zero”) can potentially have a worldwide impact.
What is not widely known to the general public is that, annually, infectious (and parasitic) diseases are the second leading cause of death (26% – 14 million) following cardiovascular diseases (29% – 16 million). Of the 14 million deaths, 6 million are from respiratory infections (global data from 2014). Put into perspective, 14 million translates into 1,600 deaths every hour – or 27 people every second.
… infectious (and parasitic) diseases are the second leading cause of death (26% – 14 million) following cardiovascular diseases (29% – 16 million).
Armed with this new knowledge of infectious diseases, let us focus on one of the methods used to contain its spread: hand disinfection. Many of us rarely leave the house without a small bottle of disinfectant in our pockets. It has become second nature; however, have you ever wondered how disinfectants were discovered to control infectious diseases? (Hint: it was not Joseph Lister.)

Ignaz Semmelweis, 1860 – Copper plate engraving by Jenő Doby – Public Domain Image
The correct answer involves a fascinating (and tragic) story with a Hungarian physician named Ignaz Philipp Semmelweis (1818-1865). He studied Medicine at the University of Vienna and worked in a charity maternity hospital. The hospital was divided into two clinics: the first staffed by midwives and the second with medical students. The latter’s medical education involved assisting with autopsies in the hospital’s morgue. Unthinkable – within today’s hospital protocols – the medical students examined the patients in labour without wearing any protective clothing or gloves.
Not surprisingly, Semmelweis noticed that women to assigned medical students suffered twice the mortality rate of “child-bed fever” (today known as puerperal sepsis – a staphylococcal infection) than those attended to by midwives.
During Semmelweis’ tenure, a medical student accidentally lacerated the hospital pathologist’s skin during an autopsy. Unfortunately, the pathologist died from this injury. Upon examination, his post-mortem was identical to the mothers that died from child-bed fever.
‘… Semmelweis noticed that women to assigned medical students suffered twice the mortality rate of “child-bed fever”… than those attended to by midwives.’
This incident led Semmelweis to postulate that the pathologist died of “particles” from the cadavers entering the vascular system. More importantly, when pregnant women were examined with hands containing these particles, this increased the probability of their absorption into the patient’s vascular system. In addition, with the patients assigned to one of two wards (medical students and midwives), the latter would not be exposed to this source of infection.
Semmelweis analyzed these findings and hypothesized that if one destroyed these particles chemically, the incidence of child-bed fever would be reduced. As such, in 1847, he implemented a regime of hand disinfecting using a solution containing chlorine. It did not take long to support his hypothesis as the maternal mortality rate dropped precipitously.
The story, however, does not end at this point. Little did Semmelweis know that he had upset the medical status quo of his day. In fact, upon learning of his findings, the Viennese College of Professors summarily cancelled his clinical appointment.
Returning to Budapest Semmelweis established a private clinic while publishing a book containing his findings. The European medical profession “old guard” rejected his published findings as a personal affront on their clinical practice. To be fair, germ-theory, the understanding that organisms too small for the naked eye causing diseases, was not accepted until nearly 30 years after Semmelweis’ work. Younger doctors, however, embraced his ideas and by 1863 hand disinfecting was a standard protocol in every Hungarian hospital.
‘The European medical profession “old guard” rejected his published findings as a personal affront on their clinical practice… germ-theory… was not accepted until nearly 30 years after Semmelweis’ work.’
The story now has a tragic ending. Semmelweis’ wife, concerned about his state of mind, had him committed under questionable medical advice into an insane asylum. He died there at the age of 47 from injuries suffered from the orderlies. His medical records were sealed by Viennese officials until they were discovered in their archives in the late 1970s. It appears he was beaten repeatedly, placed in a straightjacket and left to die without any medical attention.
A tragic end to a visionary medical professional who devoted his life’s work in changing the accepted medical paradigm of the causation of infectious diseases.
Today, 140 million births occur on an annual basis, worldwide, and those in a hospital setting have Semmelweis looking over their shoulders keeping them safe. In fact, one takes “routine births” for granted.
Finally, Semmelweis’ findings are the reason we wash our hands and use over the counter disinfectants – keeping ourselves, others and the entire world safe from the explosive effects of infectious diseases.
For those interested in Semmelweis’ work, there is an excellent review article by Nicholas Kadar, Rediscovering Ignaz Philip Semmelweis (1819-1865), in the American Journal of Obstetrics & Gynecology, January 2019.
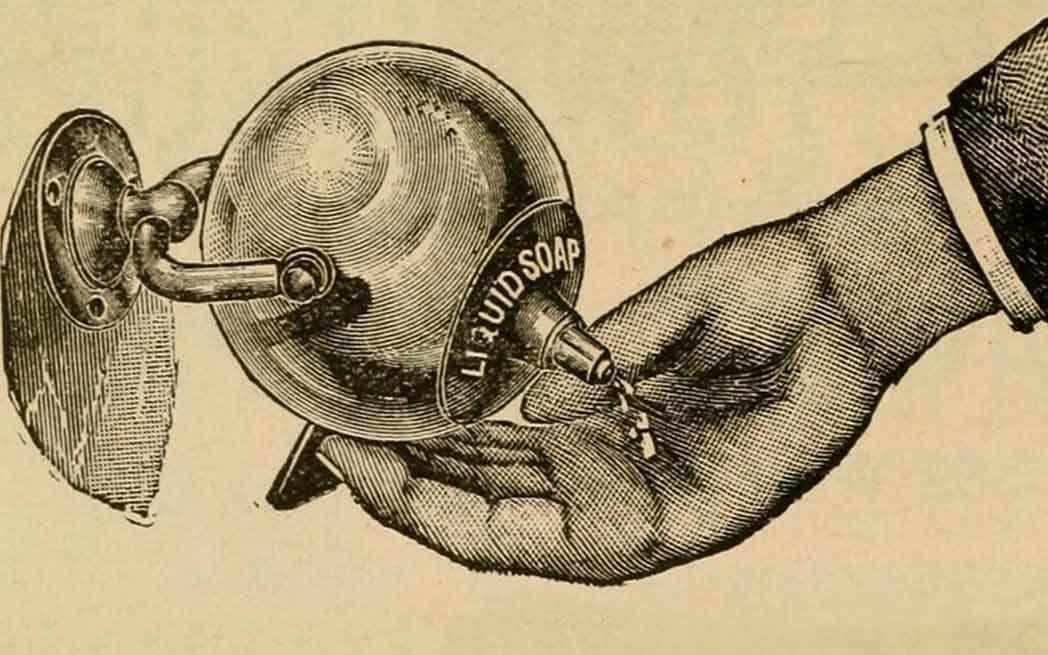
Feature image: Internet Archive Book Images via StockPholio.net
 Read also: other articles by Michael Walsh
Read also: other articles by Michael Walsh

Michael Walsh is a long-time Westmount resident. He is happily retired from nearly four decades in the field of higher education technology. A “professional student” by nature, his academic training, and publishing, include statistical methodology, mycology and animal psychology. During this period, he was also an officer in the Canadian Armed Forces. Prior to moving to Montreal, he was contracted by the Ontario Ministry of Education evaluating bilingual primary and secondary school programs. Today, he enjoys spending time with his (huge) Saint Bernard while discovering the city’s past and sharing stories of the majestic trees that grace the parks and streets. He can be contacted at michaelld2003 @hotmail.com or through his blog Westmount Overlooked


 March 10, 2026" />
March 10, 2026" />
 in shades of the Caucasus" />
in shades of the Caucasus" />
 Oriental musical poetry" />
Oriental musical poetry" />
 never seen before" />
never seen before" />
 My work here is done" />
My work here is done" />

 Purchase process in 2026" />
Purchase process in 2026" />
 as the climate changes" />
as the climate changes" />
 and business goals" />
and business goals" />
 Winchester Avenue" />
Winchester Avenue" />
 Scorched eggplant" />
Scorched eggplant" />
 Michael Hawkes /99" />
Michael Hawkes /99" />
 the world of a stray whale" />
the world of a stray whale" />
 Selling process in 2026" />
Selling process in 2026" />

 Emotional Intelligence" />
Emotional Intelligence" />
 Lemon blueberry sauce cake" />
Lemon blueberry sauce cake" />
 Kitchener Avenue" />
Kitchener Avenue" />
 where water meets fire" />
where water meets fire" />
 Market process in 2026" />
Market process in 2026" />
 and resilient leadership" />
and resilient leadership" />
 to rules–based trade" />
to rules–based trade" />

 Crunchy Asian Slaw" />
Crunchy Asian Slaw" />
Fascinating and very sad. The context is most informative.